A Professional Networking Site for Doctors & Medical Students Worldwide
Replies to This Discussion
-
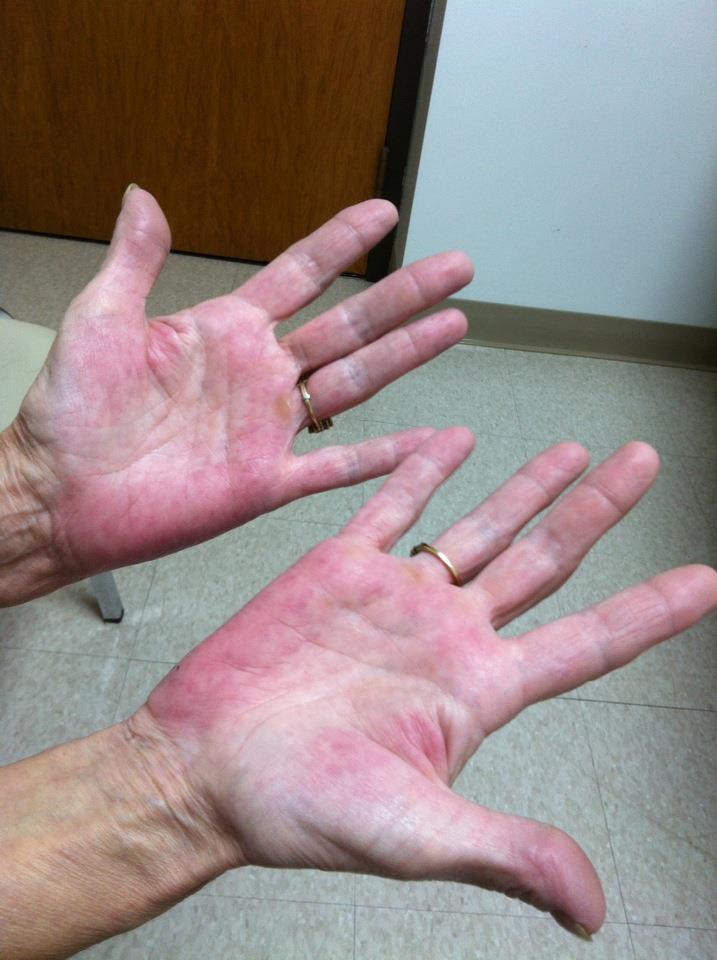
The correct answer is Palmar Erythema.
Palmar erythema (PE), an often overlooked physical finding, is due to several physiologic or systemic pathologic states. Blotchy erythema, most noticeable over the thenar and hypothenar eminences and on the tips of the fingers, is also noted in patients with chronic liver disease. This may be due to vasodilation and increased blood flow. PE can exist as a primary physiologic finding or as a secondary marker of systemic pathology.
Primary or physiologic PE can be due to heredity, occurs in at least 30% of pregnant women as a result of associated alterations in the function of the skin and its microvasculature, or may be a diagnosis of exclusion (i.e. idiopathic PE).
Secondary PE from systemic pathology encompasses a wide range of disease states. Twenty-three percent of patients with liver cirrhosis, from varying causes, can manifest PE as a result of abnormal serum estradiol levels. Patients with a rare neonatal liver disease such as Wilson disease and hereditary hemochromatosis may exhibit PE along with the other systemic manifestations of the genodermatoses. PE has been reported to occur in >60% of patients with rheumatoid arthritis and is associated with a favorable prognosis. Up to 18% of patients with thyrotoxicosis and 4.1% of patients with diabetes mellitus can have PE. This cutaneous manifestation of diabetes occurs more often than the more classic diseases such as necrobiosis lipoidica diabeticorum (0.6%). PE can be seen in early gestational syphilis and among patients with human T-lymphotrophic virus-1-associated myelopathy. Drug-induced PE with hepatic damage has been documented with use of amiodarone, gemfibrozil, and cholestyramine, while topiramate and albuterol (salbutamol) have been reported to cause PE in the setting of normal liver function. Fifteen percent of patients with both metastatic and primary brain neoplasms may have PE. Increased levels of angiogenic factors and estrogens from solid tumors have been postulated as the cause of PE in such cases. Erythema ab igne can mimic PE, and patients with atopic diathesis are more likely to have PE than matched control subjects. Smoking and chronic mercury poisoning are environmental causes of PE.
No treatment of primary PE is indicated. If medication is the cause of PE, the drug responsible should be discontinued if possible. Identification of PE related to underlying disorders should be followed by treatment of the underlying condition.
Ref : Am J Clin Dermatol. 2007;8(6):347-56.
-
Thank you Dr.Karuturi.
-
if we suspect chronic liver disease as a cause of palmar erythema we should also look for duputryen's contracture, leuconychia, clubbing, hepatic flap, jaundice, central cyanosis, parotid swelling, gynaecomastia, spider naevi, loss of hair on chest in males.
-
Palmar Erythema ?
-
Palmar Erythema with Dupuytren's Contracture of Right Third Finger.
-
palmar erythema
-
palmar erythema
-
Palmar erythema
-
Palmar erythema
- ‹ Previous
- 1
- 2
- Next ›
© 2014 Doctors Hangout | About DH